The medical billing outsourcing market is on the surge. According to the research by Reportlinker, it is expected to grow from $2.17 billion in 2021 and reach 20 billion by 2026 with an annual growth rate (CAGR) of 11.5%. The reason for this rise? Companies are resuming their operations, adapting faster than ever before after COVID-19 impacted all aspects. This includes social distancing practices such as remote working or even closure of commercial activities leading up until the early 2020s when containment measures were put into place later. It allowed some flexibility again but at a more economical cost which resulted in tough challenges faced during the recovery period.
What are those challenges, and why do DME providers choose to outsource DME billing or implement modern solutions for the revenue cycle process improvement? Let us have a closer look.
1. Labor Shortage
The high demand for labor has caused significant challenges in recent years. With businesses of all types fighting to hire new staff, retaining employees is more critical than ever! Durable medical equipment providers are not strangers when it comes to hiring and training people; they know how complicated this industry can be with its constantly changing requirements. Many DME suppliers simply don’t have enough workers available so that everything gets done on time without delays or disruptions, especially regarding billing and revenue cycle management.
2. Inefficient Systems and Processes
Relying on inefficient processes, including manual tasks, paper, and disparate systems, can not only overcomplicate operations but leads to cumbersome and error-prone billing and revenue cycle management processes. In many cases, these inefficiencies require DME providers to add staffing to meet the workload demands, which in turn increases overhead and reduces profitability.
As a result, they need to invest more time and effort into back-office work instead of focusing on client service and strategic development.
3. Lack of Knowledge
Commercial and government payers don’t make billing DME-related claims easy. With varying payer requirements, including documentation, compliance, and EDI transmission protocols – billing DME claims can be quite confusing. From prior authorizations, HCPCS and modifier combinations to state Medicaid waivers, how do providers maintain the most UpToDate knowledge base? It’s no surprise that many claims contain errors.
Eventually HME/DME companies should choose what is better for them in terms of financial opportunities and the available solutions on the market: to outsource their billing and revenue cycle processes or implement an HME/DME software such as NikoHealth. Anyway, the bottom line: Improving your revenue cycle process increases the profitability of your business.
Both approaches – outsourcing and specialized software have their pros and cons. We tried to collect most of the issues into a single comparison infographic that will help you in your decision-making.
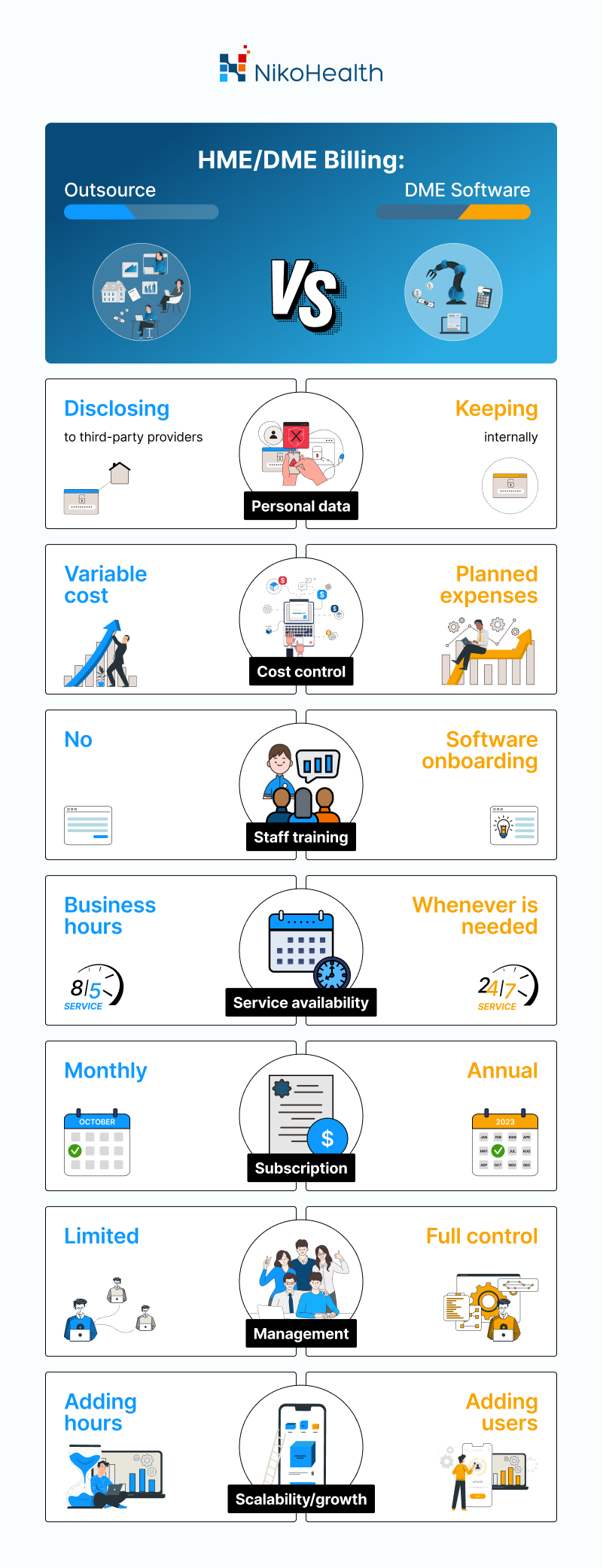
The decision to outsource may provide value, however starting with improving the front-end operations to help bridge your operational workflow gaps will prevent rejections and denials, reduce time-consuming follow-ups on accounts receivable and eliminate labor-intensive tasks.
Explore the right systems to bring all your work into one place where waste is eliminated, resulting in cleaner claims while decreasing the time and cost of getting paid.
Take control of your DME operations while reducing operational costs for claims management and speed up collections with the latest DME software to help with:
- Patient and Order Management
- Insurance Eligibility and Verification
- Simplified Patient Collections
- Inventory and Delivery
Are you ready for the next step and stand out from your competition? Discover your opportunities for growth with NikoHealth – an innovative software solution created for HME/DME professionals that connects your operations and improves your bottom line and DME billing.







Related Articles