Durable Medical Equipment (DME) billing is a complex process prone to errors and compliance challenges. In fact, studies show that about 80% of medical bills contain errors, and DME providers have an error rate of 27.4% – the highest among healthcare provider types.
These mistakes lead to financial losses and delayed reimbursements. To tackle these issues, many DME suppliers are turning to automation, which is a must to streamline operations, get paid faster, reduce denied claims, and allow staff to focus more on patient care.
Below, we outline five best practices to make the most of DME medical billing automation in your organization.
1. Standardize Documentation and Coding Processes
Successful DME medical billing automation starts with a strong foundation: accurate and standardized documentation and coding. No amount of automation can compensate for poor data quality.
Ensure your team consistently collects all required paperwork (physician orders, Certificates of Medical Necessity, etc.) and uses correct codes for each item and diagnosis. Precision in documentation and coding is essential for reducing claim denials. Small errors (like missing modifiers or incorrect HCPCS codes) can lead to rejections and denials even if you have automated systems in place.
By leveraging the automated billing rules engine, you no longer need to training you staff of DME billing procedures and coding guidelines. Your focus is now on ensuring your payor rules are updated, and let the system apply the rules.
💡 Key takeaway: This best practice lays the groundwork so that when you deploy DME billing automation, the system can process clean claims without being tripped up by avoidable errors.
2. Automate Insurance Eligibility and Authorization Checks
One of the most effective ways to prevent claim issues is to verify patient insurance before delivering DME. Manually checking each patient’s eligibility is tedious and slow, but this is exactly where DME billing automation shines.
Implement automated eligibility verification tools that connect directly to payer databases to confirm coverage and policy requirements in real time. This up-front automation ensures you only proceed with orders that will be covered, and it flags any need for prior authorizations early.
Verifying patient benefits before dispensing equipment dramatically reduces billing errors and surprises. Studies note that real-time eligibility checks and obtaining necessary authorizations in advance help prevent downstream denials. In practice, this means fewer unpaid claims, non-reimbursable inventory dispensed and less wasted effort.
💡 Key takeaway: By automating eligibility and authorization workflows, DME providers can create a smoother process from intake to billing, resulting in fewer denied claims and faster approvals.
3. Invest in DME Medical Billing Automation Solutions
Choosing the right software is critical for effective DME medical billing automation. An all-in-one DME billing software can unify your operations (from orders and inventory to claims and collections), eliminating duplicate data entry and human errors. Investing in dependable billing software significantly reduces manual mistakes and improves claim accuracy.
Modern DME billing systems include automation features that streamline key processes: they automatically verify insurance eligibility, track authorizations, submit electronic claims, and even monitor claim status in real time. Look for a cloud-based solution that integrates with your other systems (like EHRs or inventory management) to ensure seamless data flow.
The software should offer configurable rules and workflows that enforce payer requirements (such as Medicare’s documentation or frequency guidelines) and catch errors before submission.
By adopting a specialized DME billing automation tool, providers can accelerate their cash flow and reduce the cost to collect, all while minimizing the learning curve for staff with an intuitive interface.
💡 Key takeaway: The right software serves as the backbone of your automation strategy, enabling your team to work smarter, not harder.
4. Implement Intelligent Claims Scrubbing and Denial Management
Even with perfect preparation, some claims will have issues – but automation can drastically improve your clean claim rate. A best practice in DME billing automation is to use intelligent claims scrubbing tools that automatically check each claim for errors or missing information before it’s submitted.
Automated billing systems can apply payer-specific rules, ensure required documentation is attached, verify modifiers, and flag anything that doesn’t comply with billing guidelines. By catching mistakes upfront, providers see far fewer denials. In fact, real-time claim edits and scrubbing allow errors to be corrected prior to submission, resulting in fewer denied claims and faster payments.
Additionally, leverage automation for denial management: set your software to alert staff immediately when a claim is denied or pending so they can follow up. Promptly investigating and correcting denials keeps your revenue flowing.
DME billing software can automatically post payer remittances, generate secondary claims, and even bill patients once insurance has paid, reducing manual touchpoints. The goal is a proactive, closed-loop process: submissions go out clean, and any rejections are handled quickly and systematically.
💡 Key takeaway: With higher clean-claim rates and speedy follow-ups, providers often see reduced accounts receivable days and spend far less time chasing payments.
5. Leverage Analytics and Continuous Improvement
Automation isn’t a “set and forget” solution – it’s an ongoing cycle of improvement. The best DME billing automation systems come with robust analytics and reporting tools that give you deep visibility into your revenue cycle. Take advantage of these features.
Track key performance indicators (KPIs) such as denial rates, days sales outstanding (DSO), clean claim percentage, and reimbursement turnaround time. Automated systems can capture extensive billing data and generate reports on collections, common denial reasons, outstanding balances, and more. Regularly reviewing these reports will help you spot trends or problem areas.
For example, if a particular payer has rising denials for a certain code, you can investigate and adjust your processes (or update your software’s rules) accordingly. Continuous monitoring enables data-driven optimizations, ensuring your billing process gets more efficient over time.
Additionally, keep your team and software up-to-date with the latest regulations and payer policies. Healthcare rules for DME (Medicare guidelines, HCPCS code changes, etc.) evolve frequently. Make it a practice to conduct periodic audits and training sessions so that your staff and your automation rules stay current.
💡 Key takeaway: This combination of analytics and education creates a feedback loop: insights from the data inform improvements, and well-trained staff can leverage the software to its full potential. In essence, you should use the intelligence from your DME billing automation platform to continually refine your operations and maintain compliance.
How NikoHealth Can Help with DME Billing Automation
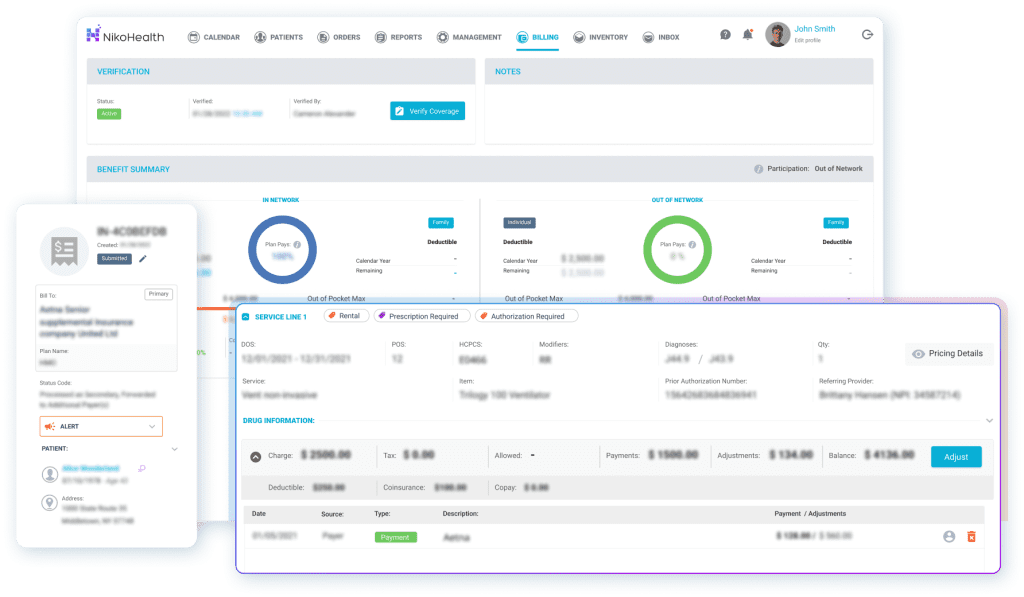
Implementing the above best practices is much easier with the right partner. NikoHealth offers an all-in-one HME/DME software platform designed to automate and streamline the entire billing process.
As a cloud-based solution, NikoHealth brings together order management, inventory, documentation, and billing into one intuitive interface, which boosts productivity and eliminates many manual touchpoints. Here’s how NikoHealth can help you put DME billing automation into action:
Intelligent Claims Management
NikoHealth’s billing software ensures every claim is clean and error-free before submission. The system automatically scrubs claims against payer rules and fills in data-driven details, so you catch mistakes in advance.
It will even automatically post payer remittances, bill any patient responsibility, and submit recurring rental invoices – significantly reducing manual work in the claims cycle. By automating claims and denials management, providers see faster reimbursements and fewer back-and-forth corrections.
Integrated Eligibility Checks
With NikoHealth, eligibility verification is built right into the workflow. The software automatically checks a patient’s insurance eligibility (and benefit coverage) before order fulfillment and prior to claim submission, helping to prevent denials and write-offs.
This real-time integration means your team won’t accidentally dispense equipment without approval, and you can be confident each claim meets payer requirements from the start.
Patient Billing and Collections
NikoHealth also automates the patient financial side of DME billing. It can generate clear patient responsibility estimates upfront and send integrated e-statements for any balance due.
The platform supports seamless collection of patient payments – whether via credit card in person, over the phone, or out in the field – all recorded in the system. By personalizing and automating the patient billing experience, you can improve collection rates and minimize delays in payment.
Analytics and Compliance
The software comes with robust analytics dashboards and reporting tools that give you real-time insight into your operations. You can track billing performance metrics, identify trends (like frequent denial reasons), and make quick decisions to optimize your process.
NikoHealth’s rules engine also helps you customize complex payer requirements (such as compliance documents or frequency limits) so that your billing stays compliant with the latest guidelines. In short, the platform not only automates tasks but also helps you enforce best practices and adapt to changes with ease.
Conclusion
By embracing a comprehensive approach to DME billing automation, providers can significantly improve revenue performance, streamline collections, and reduce the overall cost to collect. An integrated, all-in-one system minimizes disconnected workflows and eliminates many of the manual processes that often lead to errors and delays.
When automation is implemented thoughtfully, DME organizations gain better visibility into their revenue cycle, reduce administrative burden, and improve claim accuracy. This operational efficiency allows teams to spend less time correcting mistakes and more time focusing on strategic growth and patient service. Ultimately, modern DME billing automation is not just about faster claims – it’s about building a scalable, compliant, and financially resilient organization.
Frequently Asked Questions about DME Billing Automation
What is DME billing automation?
DME billing automation refers to the use of software tools and technology to handle repetitive, manual tasks in the billing process for durable medical equipment suppliers. This includes automatically verifying patient insurance eligibility, submitting electronic claims, scrubbing claims for errors, posting payer remittances, managing denials, and generating patient statements.
By automating these workflows, DME providers can reduce human error, accelerate reimbursements, and free staff to focus on higher-value tasks.
Why is DME billing more complex than other types of medical billing?
DME billing involves a unique combination of challenges not found in other billing specialties. Providers must navigate payer-specific HCPCS coding requirements, Certificates of Medical Necessity (CMNs), prior authorization rules, rental vs. purchase billing structures, frequency and quantity limits, and compliance documentation (especially for Medicare and Medicaid).
These layers of complexity contribute to DME providers having the highest claim error rate among all healthcare provider types – 27.4% – making automation especially valuable in this sector.
How does automation reduce claim denials?
Automation reduces claim denials through several mechanisms. First, real-time eligibility verification ensures coverage is confirmed before equipment is dispensed. Second, built-in claims scrubbing tools check for missing modifiers, incorrect codes, and documentation gaps before submission.
Third, automated denial tracking alerts staff promptly when a payer rejects a claim so it can be corrected and resubmitted quickly. Together, these features can reduce billing errors by up to 60% compared to manual processes.
What features should I look for in DME billing automation software?
When evaluating DME billing automation solutions, prioritize the following capabilities:
- Real-time insurance eligibility verification integrated directly into the order workflow
- Intelligent claims scrubbing with payer-specific rules engines
- Electronic claim submission and automated remittance posting
- Denial management workflows with automated alerts and tracking
- Patient billing and e-statement delivery
- Analytics dashboards for KPI tracking and denial trend analysis
- EHR and inventory system integrations for seamless data flow
- Cloud-based deployment for accessibility and scalability
Will automation replace my billing staff?
No – DME billing automation is designed to augment your staff, not replace them. Automation handles repetitive, rule-based tasks (like eligibility checks, claim scrubbing, and remittance posting) so your team can focus on exception handling, patient relationships, payer negotiations, and complex denial resolution.
Most providers find that automation allows existing staff to process significantly higher claim volumes without adding headcount, improving overall productivity and job satisfaction.
How long does it take to implement DME billing automation software?
Implementation timelines vary depending on the size of your organization, the complexity of your payer mix, and how many systems need to be integrated. Smaller DME providers using an all-in-one platform can often go live within a few weeks, while larger organizations with multiple locations or legacy system integrations may require two to four months.
Most vendors provide onboarding support, data migration assistance, and training to minimize disruption during the transition.
How does DME billing automation handle Medicare compliance?
Leading DME billing automation platforms include built-in Medicare compliance
rules that enforce documentation requirements, HCPCS coding standards, frequency and quantity limits, and CMN validation. The system’s rules engine can be updated as CMS guidelines change, ensuring your claims always reflect the latest regulatory requirements.
This is particularly important given that 1 in 4 DME suppliers faces a Medicare audit annually – having an automated compliance layer provides a critical safety net.







Related Articles