- HME and DME aren't the same thing — but they're rarely separate. HME describes the home-delivery business model; DME is the Medicare billing classification. Most providers operate both, which is why the industry shorthand HME/DME exists — and why billing teams need to understand both to avoid claim denials.
- Getting the classification wrong has real revenue consequences. Products that don't meet CMS's DME durability criteria get denied on first submission. With documentation errors (incomplete CMNs, wrong HCPCS codes) among the top denial triggers, clean claims start with knowing exactly what category your equipment falls into.
- The HME/DME market is growing faster than most providers' systems can keep up with. An aging U.S. population and the shift toward home-based care are expanding demand across mobility, respiratory, and diabetes supply categories — putting pressure on billing, inventory, and delivery workflows that many providers still manage across disconnected tools.
If you work in home healthcare or durable medical equipment supply, you’ve almost certainly seen the terms HME and DME used interchangeably — sometimes in the same sentence. For billing teams and operations managers, the distinction matters more than it might seem. Insurance reimbursement rules, Medicare coverage criteria, and supplier accreditation requirements can all hinge on how a product is classified.
This guide explains what HME means, how it relates to DME, and why understanding the overlap (and the differences) is important for any provider managing equipment, billing, and compliance.
What Is HME?
💡 HME stands for home medical equipment — a broad category of medical devices and supplies prescribed for use in a patient’s home. HME includes anything from hospital beds and wheelchairs to oxygen concentrators and CPAP machines. The defining characteristic is that it serves a therapeutic function in a non-clinical setting.
HME meaning in practice: it describes the supply model as much as the product category. An HME provider is a supplier that sources, delivers, sets up, and maintains medical equipment for patients at home, handling everything from insurance verification to Medicare billing, delivery scheduling, and ongoing resupply.
What Is DME?
DME stands for durable medical equipment. Medicare defines DME as equipment that is medically necessary, can withstand repeated use, is primarily used for a medical purpose, is generally not useful to someone who isn’t sick or injured, and is used in the home. The definition comes directly from CMS and shapes how products are billed and reimbursed under Medicare Part B.
Common DME examples include:
- Wheelchairs and scooters
- Hospital beds
- Walkers, crutches, and canes
- Infusion pumps
- supplies
DME is a regulatory and billing category defined by payers, particularly Medicare and Medicaid. To bill for DME, a supplier must hold a DMEPOS supplier number (PTAN) and meet the National Supplier Clearinghouse (NSC) accreditation standards.
HME vs DME: What’s the Difference?
The honest answer is that HME and DME overlap significantly. In day-to-day operations, most suppliers use the terms interchangeably, and many companies include both in their name (HME/DME) precisely because they serve the same patient population with the same equipment.
The practical distinction comes down to context:
| HME | DME | |
| Stands for | Home Medical Equipment | Durable Medical Equipment |
| Defined by | Industry usage and business model | CMS/Medicare regulatory criteria |
| Primary use | Equipment delivered and used at home | Equipment meeting Medicare durability criteria |
| Billing category | Not a specific billing code category | Formal billing category under Medicare Part B |
| Accreditation | ACHC or BOC accreditation required | DMEPOS accreditation required to bill Medicare |
| Who uses the term | Suppliers, industry professionals | Medicare, payers, billing/compliance teams |
💡 In practical terms: all DME that is used at home falls under HME — but HME as a concept is broader, covering the business model, delivery logistics, and patient relationship, not just the product specifications that qualify for reimbursement.
Why the HME/DME Distinction Matters for Billing and Operations
For HME/DME providers, the HME vs DME terminology is more than semantics — it has direct implications for how you set up billing workflows, structure your compliance program, and manage your product catalog.
Medicare Reimbursement Rules
Products that qualify as DME under Medicare Part B must meet CMS’s definition precisely to be eligible for reimbursement. An item that doesn’t meet the durability or medical necessity criteria will be denied — regardless of how it’s labeled internally. Billing teams need to understand which products qualify as DME and ensure claims are submitted with the correct HCPCS codes and supporting documentation, including a Certificate of Medical Necessity (CMN) where required.
📖 For a detailed breakdown of how Medicare billing works for DME suppliers, see our guide to DME billing.
DMEPOS Accreditation Requirements
To bill Medicare for DME, suppliers must be accredited through a CMS-approved organization — either BOC or ACHC. Accreditation verifies that the supplier meets standards for quality, storage, delivery, and patient safety. This applies whether you describe your business as an HME or DME provider — the regulatory requirement is the same.
📖 Keep current with DME compliance updates to stay ahead of accreditation and regulatory changes.
Claim Denial Management
Many claim denials stem from incorrect product classification — billing a non-durable item as DME, or missing required documentation for a specific HCPCS code. A structured revenue cycle management process with automated pre-submission checks helps catch these errors before they reach the payer.
Common HME/DME Product Categories
Most HME/DME providers manage a mix of product categories that span both simple and complex equipment. Here’s how the main categories break down:
- Mobility Equipment Wheelchairs (manual and power), scooters, walkers, crutches. Typically billed as capped rental or lump-sum purchase under Medicare.
- Respiratory Equipment Oxygen concentrators, CPAP, BiPAP, nebulizers. Often involves recurring rental billing and resupply schedules.
- Hospital Beds and Accessories Adjustable beds, pressure-relief mattresses, bed rails. Require CMN documentation and medical necessity criteria.
- Diabetes Supplies Blood glucose monitors, test strips, lancets. Subject to competitive bidding program pricing in many regions.
- Orthotics and Prosthetics (O&P) Braces, prosthetic limbs. Governed by additional CMS rules and often requires separate accreditation.
- Home Infusion IV therapy, parenteral nutrition. Falls under a separate Medicare benefit category from standard DME.
Managing this breadth of product types — each with different billing rules, rental vs. purchase classifications, and documentation requirements — is one of the core operational challenges for HME/DME suppliers.
📖 See our related guide: what is a DME provider and how to become one.
How HME/DME Providers Manage Operations
Running an HME/DME business involves coordinating several functions simultaneously — often with different systems for each. Providers handle:
- Patient intake: Collecting insurance information, verifying coverage, and processing physician orders and CMN documentation.
- Inventory management: Tracking stock levels, managing serialized assets, and maintaining service and maintenance records for rental equipment.
- Order and delivery management: Processing orders, routing deliveries, capturing e-signatures, and coordinating returns and exchanges.
- Billing and RCM: Submitting clean claims, managing denials, processing ERA/EOB remittances, and handling recurring rental invoicing.
Historically, many providers run separate systems for each of these functions — billing software, an inventory spreadsheet, a delivery log. That fragmentation creates data gaps, billing errors, and slow collections.
Modern DME inventory management software and all-in-one platforms now consolidate these functions into a single system, reducing manual work and giving providers real-time visibility across operations.
📖 If you’re evaluating whether to outsource or manage billing internally, this guide on DME billing outsourcing vs. in-house can help you weigh the trade-offs.
What to Look for in HME/DME Software
The right software platform for an HME/DME business does more than process claims. It needs to handle the full operational lifecycle — patient intake, order management, inventory, delivery, and revenue cycle — without requiring providers to stitch together multiple disconnected tools.
Key capabilities to evaluate:
- Automated eligibility verification at intake — catch coverage issues before they become denials
- Claims scrubbing and denial management — pre-submission compliance checks built into the workflow
- Recurring rental billing automation — critical for oxygen, CPAP, and other capped rental equipment
- Real-time inventory visibility — serialized asset tracking, service history, reorder alerts
- Mobile delivery app — e-signatures, delivery confirmation, and real-time field-office sync
- ERA/EOB remittance posting — automated posting eliminates manual data entry across hundreds of payer remittances
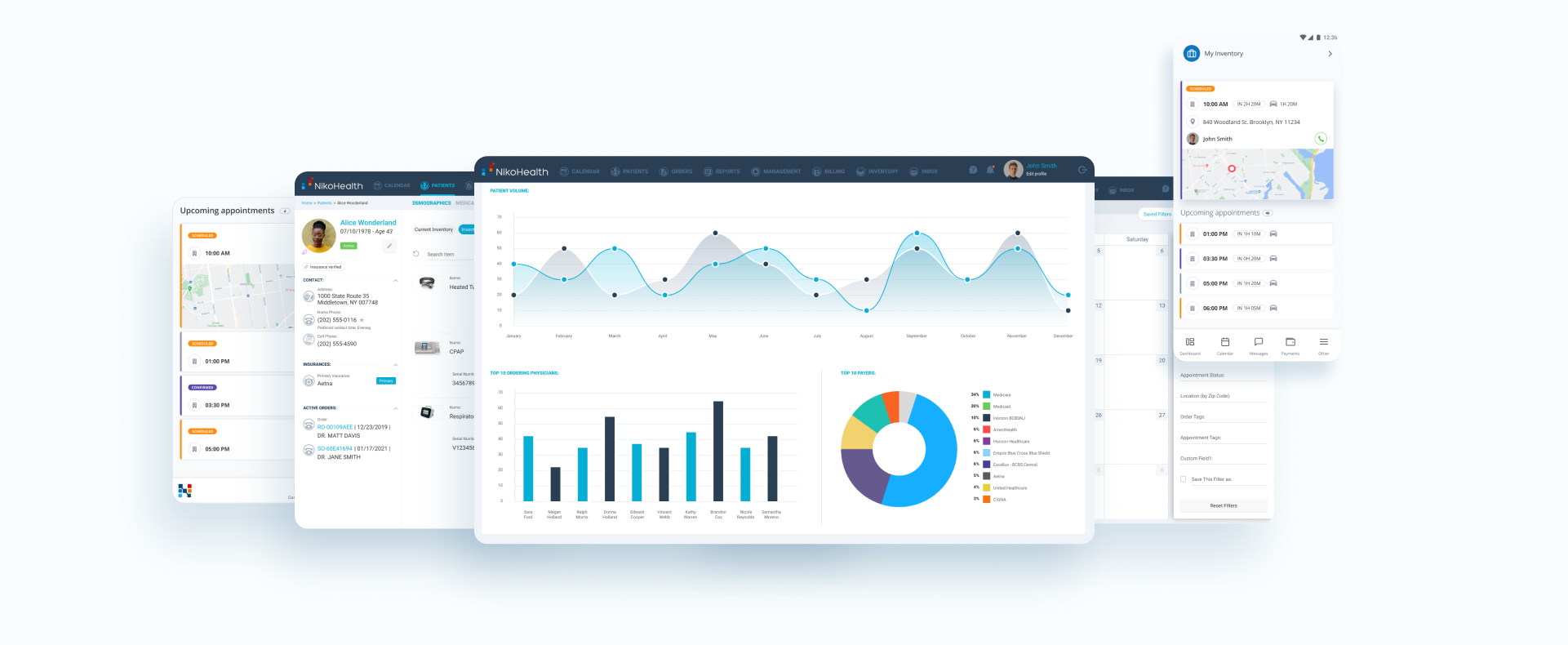
NikoHealth’s HME/DME billing software and RCM software are purpose-built for this environment — consolidating billing, inventory, delivery, and revenue cycle management in one platform designed exclusively for HME/DME providers.
Frequently Asked Questions: HME vs DME
What does HME stand for?
HME stands for home medical equipment. It refers to medical devices and supplies prescribed for use in a patient’s home, including wheelchairs, oxygen equipment, hospital beds, and CPAP machines. HME describes both the product category and the provider model — companies that supply, deliver, and maintain equipment for home-based patients.
What is the difference between HME and DME?
DME (durable medical equipment) is a regulatory category defined by Medicare and CMS — it sets the criteria a product must meet to qualify for reimbursement. HME (home medical equipment) is a broader industry term that describes equipment used at home and the business model around delivering it. Most products that qualify as DME for billing purposes also fall under the HME umbrella. The terms are often used together (HME/DME) because most suppliers provide both.
Do HME and DME providers need accreditation?
Yes. To bill Medicare for DME, suppliers must complete DMEPOS accreditation through a CMS-approved organization, such as ACHC or BOC. This applies whether you identify as an HME or DME provider. Accreditation requirements cover product storage, delivery practices, patient documentation, and quality management.
What software do HME/DME providers use?
HME/DME providers typically use specialized software that manages billing, inventory, order processing, delivery, and revenue cycle management in one platform. Purpose-built solutions like NikoHealth are designed for the unique billing rules, rental models, and compliance requirements of the DME industry — unlike generic healthcare software that needs to be adapted to fit.
What is a DMEPOS supplier?
DMEPOS stands for Durable Medical Equipment, Prosthetics, Orthotics, and Supplies. A DMEPOS supplier is a business enrolled with Medicare to supply any of these product categories to patients. Enrollment requires a supplier number (PTAN), CMS-approved accreditation, and compliance with the National Supplier Clearinghouse standards.







Related Articles