- The Medicare DMEPOS fee schedule sets a payment ceiling — not a guaranteed amount. Your actual reimbursement depends on your HCPCS code, your patient's location, and whether competitive bidding rules apply.
- CMS updates the fee schedule quarterly. Billing teams that don't track these changes submit claims against outdated rate expectations, which causes collection shortfalls that are hard to trace.
- Looking up rates requires more than downloading a CMS file. You need to match the right jurisdiction, modifier, and payment category to pull the number that will actually appear on your ERA.
Most DME billing managers have run into this at least once: you check the CMS fee schedule before submitting a claim, the rate looks reasonable, and then the ERA comes back with a payment that doesn’t match. The problem usually isn’t a denial — it’s that the fee schedule number you pulled wasn’t the right one for your situation.
The Medicare DMEPOS fee schedule is not a single, universal list. It’s a layered system with different rates depending on your HCPCS code, the patient’s location, whether the item falls under competitive bidding, and how the item is categorized for payment. Understanding how it actually works — and how to look up the number that will appear on your remittance — is foundational to accurate revenue forecasting and clean claims submission.
This guide walks through how the fee schedule is structured, where to find current rates, and what factors determine what Medicare will actually pay for a specific item.
What Is the Medicare DMEPOS Fee Schedule?
The Medicare DMEPOS fee schedule is a standardized list of maximum payment amounts that CMS uses to reimburse enrolled suppliers for covered durable medical equipment, prosthetics, orthotics, and supplies under Medicare Part B. Published by the Centers for Medicare & Medicaid Services (CMS), the fee schedule is updated quarterly and covers thousands of HCPCS Level II codes.
The fee schedule sets a ceiling, not a floor. Medicare pays the lesser of the supplier’s actual charge or the applicable fee schedule amount. Once the fee schedule amount is reached, Part B pays 80% of that figure — leaving the patient responsible for the remaining 20% coinsurance after their annual deductible is met.
💡Definition: The DMEPOS fee schedule is a CMS-published list of maximum reimbursement amounts for Medicare-covered DME, prosthetics, orthotics, and supplies. Payment rates are HCPCS code-specific, geographically adjusted, and updated quarterly. Medicare Part B pays 80% of the applicable fee schedule amount after the beneficiary’s annual deductible is satisfied.
How Does CMS Determine Fee Schedule Amounts?
The calculation methodology varies depending on how an item is classified. CMS does not use a single formula across all DMEPOS products. There are three primary rate-setting mechanisms you need to know:
1. Standard Fee Schedule (Non-Competitive Bidding Items)
For items not subject to competitive bidding, CMS calculates fee schedule amounts based on historical base-year data and applies annual updates tied to the Consumer Price Index for All Urban Consumers (CPI-U), adjusted by a productivity factor. For CY 2026, CMS applied a 2.0% update factor to most non-CBP items.
Examples of non-CBP items include urological supplies, ostomy supplies, and certain orthotic products. These items follow the standard inflation-adjusted methodology regardless of where the patient lives.
2. Competitive Bidding Program (CBP) Rates
For items that have historically been subject to the DMEPOS Competitive Bidding Program — including CPAP devices, power wheelchairs, oxygen equipment, and standard wheelchairs — payment rates are based on single payment amounts (SPAs) established through competitive bids.
As of January 2024, CMS is in a gap period for competitive bidding. The Round 2021 contracts for off-the-shelf back braces and knee braces expired December 31, 2023, and CMS has not yet finalized the next round of competitive bidding. During this gap, former competitive bidding area (CBA) rates are maintained and updated annually by CPI-U. For CY 2026, items in former CBAs received a 2.8% increase.
3. Special Payment Categories
Certain item categories follow specific statutory rules:
- Oxygen equipment: Reimbursed on a monthly rental basis, capped at 36 months of continuous use, with separate payment for oxygen contents after the cap
- Capped rental items: Monthly payments up to a defined rental cap, after which the item transfers to patient ownership
- Inexpensive or routinely purchased items: Option for either lump-sum purchase or monthly rental
- Frequent and substantial servicing items: Monthly rental for items requiring ongoing technical maintenance
| Payment Category | How Rate Is Set |
| Non-CBP standard items | Base year amount + annual CPI-U adjustment (minus productivity) |
| Former CBA items (CBP gap period) | Last SPA + annual CPI-U adjustment |
| Oxygen equipment | Monthly rental per statutory formula; 36-month cap applies |
| Mail-order diabetic testing supplies | National mail-order rates; competitive bidding rules apply |
| Lymphedema compression items | Set via CMS-1780-F (2023); updated annually at 2.7% for CY 2026 |
How to Look Up DMEPOS Fee Schedule Rates
There are two primary methods for accessing current Medicare fee schedule amounts. The right approach depends on whether you need a quick lookup for a specific claim or a full rate review across your active HCPCS codes.
Method 1: CMS DMEPOS Fee Schedule Files (Direct Download)
CMS publishes quarterly fee schedule files as downloadable ZIP archives on their official fee schedule page. Each file includes:
- Fee schedule amounts (floors and ceilings) for all HCPCS codes
- Payment category indicators (e.g., purchase, rental, inexpensive/routinely purchased)
- Jurisdiction codes linking rates to geographic areas
- Competitive bidding area flags
To find the correct rate for a specific claim:
- Navigate to the CMS DMEPOS Fee Schedule Files page
- Download the file corresponding to the claim’s date of service (files are released quarterly)
- Open the fee schedule file for your DME MAC jurisdiction
- Filter by your HCPCS code and payment category
- Verify the patient’s ZIP code against the CBA Zip lookup to determine if former CBA rates apply
- Apply the correct modifier (e.g., KH for initial claim, KI/KJ for months 2–3 and 4–13 of capped rental)
Official resource: CMS DMEPOS Fee Schedule Files — updated quarterly; select the file matching the date of service.
Method 2: MAC Fee Schedule Lookup Tools
Your DME MAC (Medicare Administrative Contractor) — either Noridian (Jurisdictions A and D) or CGS (Jurisdictions B and C) — provides searchable fee schedule lookup tools that let you enter an HCPCS code and state to retrieve applicable rates without downloading a full file.
- Noridian (JA, JD): Fee Schedule Lookup Tool — enter HCPCS and state to view applicable rates.
- CGS (JB, JC): CGS Fee Schedule Search — searchable by HCPCS and jurisdiction.
MAC tools are more convenient for individual claim lookups, but note they may lag slightly behind CMS quarterly updates. For billing audits or bulk rate verification, always use the official CMS source files.
Why Your Actual Payment May Differ from the Listed Rate
Even when you’ve pulled the correct fee schedule amount for an HCPCS code, the ERA may still show a lower payment. These are the most common reasons:
Geographic Adjustment
Rates for items subject to competitive bidding vary by the patient’s location. A power wheelchair delivered to a patient in a former competitive bidding area will reimburse differently than the same item delivered to a patient in a rural non-CBA zip code. Always verify the patient’s zip code before estimating reimbursement.
Modifier Errors
DMEPOS capped rental items require specific modifiers to indicate which month of the rental cycle a claim covers. Using the wrong modifier (or omitting it) can result in reduced payment or denial. KH, KI, and KJ modifiers control how Medicare pays across the rental lifecycle.
Assignment Requirement
Enrolled DMEPOS suppliers must accept assignment on Medicare claims, meaning they agree to accept the Medicare-approved amount as payment in full. If a supplier doesn’t accept assignment on a specific claim, payment rules change. Most enrolled suppliers accept assignment as a condition of Medicare enrollment.
Sequestration
A 2% sequestration reduction has applied to Medicare fee-for-service payments since 2013. The actual payment is 98% of the calculated fee schedule amount before cost-sharing. This is automatic and applies to all DMEPOS claims regardless of item type.
Simultaneous Billing and Overlapping Supplies
Medicare will not pay for supplies billed in excess of documented medical need or during overlapping supply periods. If a patient already has an active supply of a recurring item, billing before the permitted refill window triggers a payment reduction or denial — not a fee schedule discrepancy.
Understanding Fee Schedule Updates: When Rates Change
CMS releases fee schedule updates on a quarterly cycle: January, April, July, and October. The annual update — released each December for the following calendar year — sets the CPI-U adjustment factors and addresses any policy changes affecting payment categories.
For CY 2026, CMS published the fee schedule update on December 19, 2025, with rates effective January 1, 2026. The update factors differ by item category:
- 2.0% for most non-competitive bidding items
- 2.8% for items in former competitive bidding areas
- 2.7% for lymphedema compression treatment items
Billing teams should subscribe to CMS MLN Matters articles and their MAC’s update bulletins to track quarterly changes. The HFMA DMEPOS fee schedule comparison tool provides a useful side-by-side view of 2025 vs. 2026 rates and includes a HCPCS lookup function.
The Competitive Bidding Gap: What It Means for Current Billing
The most significant structural shift in DMEPOS payment over the past two years is the gap in the competitive bidding program. With all Round 2021 contracts expired and new bidding not yet underway, billing rules for CBP items are in a transitional state.
CMS has confirmed a target implementation date of no later than January 1, 2028 for the next round of competitive bidding. Until then, former CBA rates apply and are adjusted annually. The next round is expected to include a broader set of product categories than Round 2021, with new provisions for:
- Remote item delivery (RID) competitive bidding — a national or regional CBP for items shipped directly to patients
- Continuous glucose monitors (CGMs) and insulin pumps entering competitive bidding for the first time
- Revised single payment amount (SPA) methodology to account for inflation within multi-year contracts
For the most current program status, refer to the CMS DMEPOS Competitive Bidding Program page.
How NikoHealth Supports Fee Schedule Accuracy
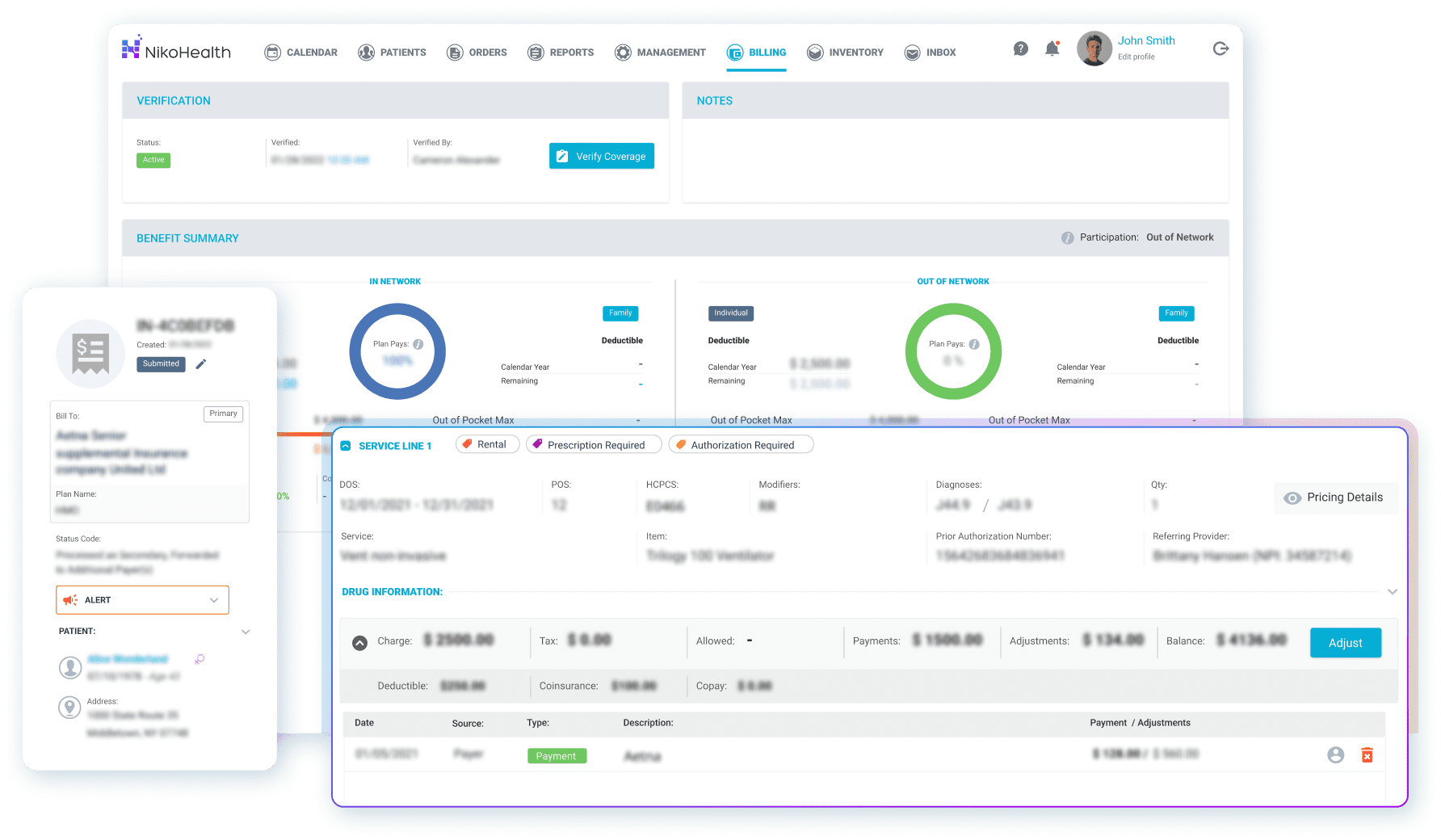
Tracking DMEPOS fee schedule rates manually — across quarterly updates, multiple jurisdictions, and item-specific modifiers — adds significant burden to billing teams that are already managing claim denials, prior authorizations, and remittance posting.
NikoHealth’s billing and RCM platform is built specifically for HME/DME providers and is designed to reduce the gap between what the fee schedule says and what your team actually collects. Key capabilities relevant to fee schedule management include:
- Automated eligibility verification at intake — confirms coverage and expected payment before service delivery
- DME claims scrubbing before submission — flags modifier errors, billing window violations, and category mismatches that cause payment discrepancies
- Automated remittance posting — processes ERA/EOB data and surfaces payment variances against expected amounts, so your team sees shortfalls rather than absorbing them
- Denial management workflows — ensures underpaid or rejected claims tied to rate mismatches are reviewed and resubmitted within timely filing windows
If your billing team is regularly finding that ERA payments don’t match rate expectations, the issue is often in the pre-submission process — not the fee schedule itself. Clean claims submitted with the correct HCPCS code, modifier, and jurisdiction data get paid correctly the first time.
To see how NikoHealth handles the DME revenue cycle end to end, explore our DME billing software overview or request a demo to walk through the platform with a NikoHealth specialist.
FAQ: Medicare DME Fee Schedule
What is the Medicare DMEPOS fee schedule?
The Medicare DMEPOS fee schedule is a CMS-published list of maximum payment amounts for covered durable medical equipment, prosthetics, orthotics, and supplies under Medicare Part B. Rates are specific to HCPCS codes, updated quarterly, and vary by geographic location and competitive bidding status.
How often does CMS update the DME fee schedule?
CMS updates the DMEPOS fee schedule quarterly — in January, April, July, and October. The annual rate adjustment for the following calendar year is published each December and sets the inflation factor applied to each payment category.
Where can I look up Medicare DME fee schedule rates?
The primary source is the CMS DMEPOS Fee Schedule Files page. Quarterly ZIP files contain rates for all HCPCS codes. Your DME MAC — Noridian or CGS — also provides searchable lookup tools. For year-over-year comparisons, HFMA publishes a fee schedule comparison spreadsheet with HCPCS-level lookup.
Why does my ERA payment differ from the fee schedule amount?
Common reasons include geographic adjustments for competitive bidding areas, incorrect rental modifiers, the 2% sequestration reduction applied to all FFS claims, or billing before the permitted refill window on recurring supply items. Verifying HCPCS codes, modifiers, and patient location before submission reduces these discrepancies.
How does competitive bidding affect DME payment rates?
For items historically subject to competitive bidding — including CPAP devices, oxygen, and power wheelchairs — rates are based on single payment amounts established through competitive bids, rather than the standard CPI-adjusted methodology. CMS is currently in a gap period (since January 2024) with a new bidding round targeted for no later than January 2028.
Does Medicare pay 100% of the fee schedule amount?
No. Medicare Part B pays 80% of the applicable fee schedule amount after the beneficiary’s annual deductible is met. The patient is responsible for the remaining 20% as coinsurance. A 2% sequestration reduction is also applied to all Medicare fee-for-service payments, so the effective Medicare payment is 78.4% of the approved amount.
 Abby Rapcienski">
Abby Rapcienski">





Related Articles